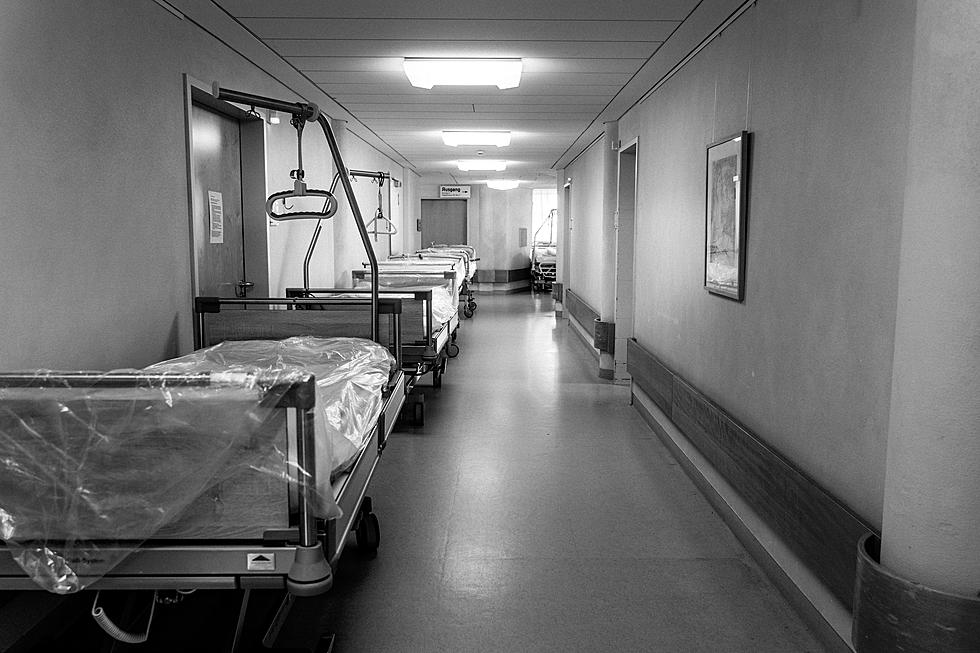
Lafayette Nurses Distraught As COVID Battle Rages
Post Traumatic Stress Disorder, exhaustion, depression, and anguish are just a few of the emotions of nurses at Ochsner Lafayette General that they were kind enough to share with me.
I am bringing you another story of nurses who are on the front line fighting COVID. This is not an article to be politicized, criticized, or critique because these are the true experiences of the people who will be there to save your life if you have an extremely bad reaction from COVID-19.
This article is meant to inform people about what it's like to be a health professional at a time when a pandemic continues, and treatment evolves. The nurses I spoke with feel as if people target them now because they are in the health care profession. It makes me sad for all of us that people can't give the same respect to a health care professional that they would give to a stranger on the street. I have never understood why people get mean when trying to share their point of view. Social media is a blessing and a curse.
I had a chance Tuesday to visit with several people at Ochsner Lafayette General so I could find out for myself what is happening with patients on their COVID floors. More importantly, COVID patients are not the only people needing life-saving care. Think about it; heart attacks don't wait until a pandemic is passed. Babies don't wait to be born. In fact, as I walked into the hospital, the code came over the loudspeakers that the Emergency Department was about to receive a stroke victim.
There are several things that the staff at Ochsner Lafayette General want to make sure people understand. If you are having an emergency, make sure you come to the hospital or call 911 for an ambulance. It was a problem early on in the pandemic, and it's a problem that persists. People are fearful of getting COVID, so they don't come to the hospital when they should. Another issue that is very important is about COVID testing. If you need to have a COVID test, please DO NOT come to the hospital. The reason? There is free COVID testing at many locations throughout Lafayette and Acadiana.
I was escorted around the hospital by Chief Executive Officer Al Patin (also a nurse) and Chief of Surgery Julie Broussard. During Tuesday's visit, Patin explained that 125 of their staff were out pending the return of COVID testing. Let that sink in. You're already overworked through four prior surges and now all of these people can't go to work because they may have COVID. Thank God there are people that are willing to risk their lives to save other people. Please, let that sink in. Don't make this post political, just understand there is a perspective that hopefully, you will NEVER have to experience first hand.
The hospital is already almost at a critical level, and yes, there is a plan to add additional space, but you know what they won't find? Nurses. There is a national nursing shortage that only intensified when the COVID pandemic. There are bidding wars for nurses going on across the state of Louisiana.
Tuesday, there were 146 people in the five of the seven facilities of the Ochsner Lafayette system that take patients with COVID. Of those, 86 with COVID were at Lafayette General, Today, there are 162 COVID patients in their system, and 98 of those patients are at LGMC. Unfortunately, officials across the state say the peak of this surge will not happen until September 1. To add to the frustration, Patin says that peak estimate DOES NOT account for what impact the state of school might have on numbers.
This is not some experience of some people we don't know. These are the people that are on the front lines of this battle, and they themselves are battling homelessness, PTSD, depression, and anguish just to point out a few of the issues. One of the nurses told me that this week a woman in her late fifties FaceTime her daughter before they intubated her because she knows the percentage of getting better after intubation is extremely low. This woman's situation is not isolated. This is happening on a regular basis. You might want to say, "Then quit!". Sounds easy for you to say, but what are you going to do when these nurses do quit because they are so burnt out? We need our nurses so instead of criticizing, please do something positive in support of nurses and other first responders.
Many people have referred to "everyone in a hospital just marking these patients down as COVID patients for the money". It's ridiculous says Chief of Surgery Dr. Julie Broussard says. What really pays the bills are everyday emergencies and people who are coming in for elective procedures, and with a hospital full to capacity, they are not doing those types of procedures. Here is another myth that Dr. Broussard would like to crush, people in the public may say, "they just mark everything down as COVID. This person I know went in with something else, and they JUST SAID it was COVID. Well, when you come in and you are extremely ill, you will be tested for COVID, and the results of the PCR tests aren't RAPID. It takes days to get official results back, so yes, you may think it's one thing and it's actually COVID. You need to check your source of information. Instead of "my friend heard, or so and so told me", call your doctor and ask them for the straight-up information about COVID.
Patin and Broussard say their nursing staff does an amazing job with the amount of stress they are under, but these surges are taking a toll on these women and men. Do you think you could sit around and listen to someone struggling to breathe? Ask yourself that question. This is the reality for these nurses each day of this surge and any day they have a COVID patient. They also want to point out that the average age of patients in this surge is 55. It's not the old and frail. Delta has changed the face of the pandemic. The average age in the prior surge was 75. Let that sink in. I saw rooms full of young adults and people through their fifties hooked up to multiple machines lying in the prone position so that they can get enough oxygen to live. Another myth to be busted? You can't just keep turning up the oxygen so that someone will live. At some point, COVID chokes off a person's capacity to breathe.
The first nurse that I spoke to one on one was the Charge nurse for the Emergency Room. All the rooms are full and some patients have been in there for two days. Candice does an amazing job of orchestrating the flow of getting people into the Emergency Room, figuring out their situation, and trying to care for them in the Emergency Department. There are no rooms on the upper floors. These ER nurses usually assess the situation, and then send them to a room. Now, they are holding them in ER and treating them. Because of privacy, one of the biggest complaints people have is they don't understand why they can't be seen right away. It's like Candice explains, you are treated as quickly as possible based on the severity of your situation. All the rooms are full, but people do not understand this, and they DEMAND a room immediately.
Candice says the reason so many nurses stick around in this fifth surge is because of the support they receive from their coworkers and Ochsner. She says the saddest thing of all happens all the time in the ER now, and that's regret. She says she has stopped counting how many times people have been in the ER now who are filled with regret for not getting vaccinated, and now, "they know it's too late". When I was there Tuesday, there were twenty-five people in rooms in the ER, and there were many more waiting in the lobby. A trip to the lobby can be a long wait as so many people are needing help. The longest a patient was in the ER was forty-four hours.
As we moved on from the Emergency Room, Dr. Broussard and Patin spoke about the "silent crisis". They are very fearful of how many people with serious issues are not seeking care because they are afraid to come to the hospital. They will downplay their symptoms, and both point out how dangerous this is. It can be deadly. Both Broussard and Patin reiterated that it is imperative that if you are having an emergency that you either come to the hospital or call 911.
The burnout among Lafayette nurses fighting the continued COVID surges is real. I got the chance to speak to Megan, one of the nurses on one of the COVID floors of LGMC. She says her patients are so gracious and kind to her. She says they are so appreciative of how she cares for them. She adds they are also often scared, and some are in denial about how bad their situation is. She says helping to keep people breathing and battling COVID is what she does every minute of every shift that she works. She says her patients need constant care as COVID is a virus that wreaks havoc on patient's systems. It has strange ups and downs when it comes to fever, heart fluctuations, and overall stress to the system.
Megan says she is one of the nurses who will take the extra shifts that are so frequently offered now that nurses are in such high demand in our state. She says Ochsner is offering very good incentives, but she says she would work anyway because she knows how badly patients need help.
One thing she would rather not have to deal with are the constant nightmares. She says almost every night her sleep is disturbed by haunting dreams. She says often it's a scenario that plays out where she can't help a patient breathe no matter what she does. This woman wakes up in a sweat. She has Post Traumatic Stress Disorder, but she carries on.
Megan says nurses are exhausted and stressed thin by the surges which invariably puts a strain on the entire hospital system. She won't stop being a nurse though as she knows it's what she is called to do. She says she does wish that more people would get the vaccine, and she says so many of her patients tell her they wish they had. She says struggling to breathe is a terrible thing for a person to experience, and patients that are battling COVID have so many obstacles. They have to be constantly monitored. They need physical therapy, occupational therapy, and even speech therapy to make sure they are still able to properly swallow so they won't choke to death.
Megan wants people to know that her patients are in their 30's, 40's and 50's. That statement is also true of Amber who works on another COVID floor at LGMC.
Amber works every day doing what she can to help her patients, and she does this even though she has an immunodeficiency. The same is true of her son. When Amber goes to work she thinks not only about the health of her patients, but also the health of herself and her child.
These nurses that serve each day are giving up so much of their lives. They are exhausted and worried. They worry for their patients and themselves. She walks into a hospital to nurse COVID sick patients knowing each day that she must do everything to protect herself so she can protect her child.
Amber is no stranger to danger either. After Hurricane Katrina, she worked helping babies in the hospital in all the mayhem that followed the storm. She told me each surge is worse than Katrina. The surges keep coming, and they are going to continue to do so because as Patin points out, there is no chance at herd immunity. It is not going to happen. He says what is going to happen is that we will continue to have surges, and so we are going to be dealing with this situation for the foreseeable future. That stark reality has left Amber and her coworkers feeling completely helpless. She worked so hard not to cry while talking to me. These people are breaking under the strain. I also see that she continues to push back the pain, numbing herself to it to continue to do her job. All these nurses do.
People have a choice, and they have to do what they feel is best, but these nurses also are doing their best to keep as many COVID patients alive as possible. They took the Hippocratic Oath. Their burden is one they choose, and what would we do without so many people willing to walk into the lion's den each day to take care of us? This virus will continue to mutate, that's what viruses do. We can argue all the points we want day after day, but it doesn't change the fact that if you are immunized against COVID and contract it, you have a ninety percent plus chance of not having to deal with major complications including death.
You may find it easy to criticize people on social media, but just remember that it's one of these nurses who will answer the call to take care of you or someone you love.
These people are putting everything on the line each day to care for people because that is how God made them; to serve. I don't understand why people choose to criticize and politicize people who are just helping others. There are plenty of other people to fight with, so please leave the first responders alone. When we first started dealing with this pandemic last year, there was a massive outpouring from Acadiana to rally around our medical professionals, but that seems to be no more, and I question why. We are a loving and graceful people who now fight with one another.
So, take away from this article what you will because that's our right as Americans. I would ask though that the ugliness leveled at medical professionals come to a halt. They are our friends, family, and they are the first line of defense.
Choose what's right for you, but understand that everything that I have presented here to you today is what these women and many other professionals are dealing with each day. I can't do what they can do. Can you? I'm very thankful someone answers the call to help because I truly believe that's what God calls us to do. Everyone has a choice.
In summation, please remember when you have an emergency, go to the hospital or call 911. When you need a COVID test, go elsewhere. And please remember that while you sit reading this someone in a hospital near you is holding the hand of someone who might die today; comforting them and willing them to be able to breathe. Let's return compassion to a subject that has divided us as a people.
Also, If you are going to visit someone with COVID, here is the latest policy on visitation:
- One (1) visitor is allowed between 4 p.m. – 7 p.m.
- For COVID-positive patients in the ICU, one (1) visitor will be allowed from 5 p.m. - 6 p.m. only.
- Visitors must remain in the patient’s room at all times, wearing appropriate PPE, which will be provided to you.
- Exceptions will be made for end of life.